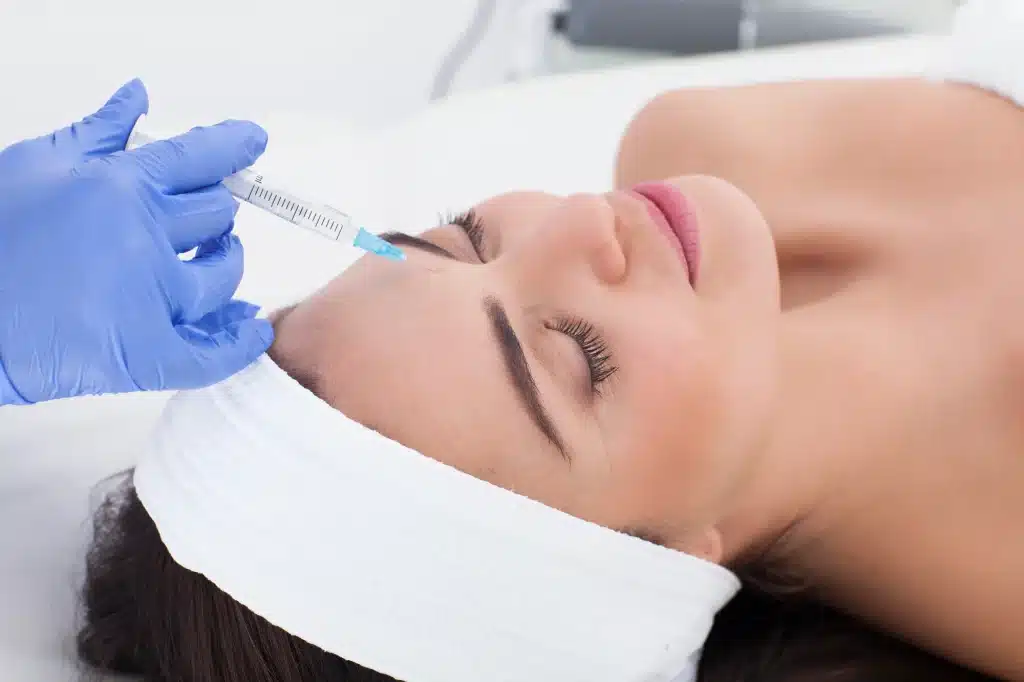
Treating and Rejuvenating Lips
The lips can be one of the prominent areas of concern for patients concerned with their aesthetic appearance. Rejuvenation of the perioral area, the area including the lips, involves correcting age-related loss of lip volume, smoker’s lines, bleeding of lipstick into the perioral rhytids, and the asymmetrical turns of the mouth. However, many patients should carefully consider aesthetic treatments for the lips, as its anatomy is delicate. Some concerns of lip treatment include the appearance of the unnatural-looking “trout pout” and the possibility of repeat treatments being required.
Two of the most popular aesthetic treatment modalities for the lips in the market right now involve the use of hyaluronic acid (HA) dermal fillers and ablative lasers, respectively. In this article, we will explore these two treatments and tips on how to avoid any problematic outcomes with them. These treatments may not be applicable to all patients, so it is very important to keep up to date with all the new products and techniques available.
Patient Analysis
The most important step prior to lip treatment, or any aesthetic treatment for that matter, is to have a proper diagnosis and evaluation session with the patient. Ideally, a successful lip augmentation is one that has minimal complications, brings about the optimal appearance, and is highly durable. To achieve this, the practitioner should identify what the patient desires at the outset and, if necessary, negotiate treatment goals so that they are more suitable for the patient’s facial contour. While some patients may have done their research and are well informed, other patients may not be fully aware of what a full treatment usually entails. Educate patients to avoid any misunderstandings and misplaced expectations on the part of patients. [1]
HA Dermal Fillers for Lips
Technically speaking, HA is the most appropriate material for the lips’ delicate and vulnerable structure. Since the lips are highly vascularized, non-HA fillers may cause complications and are not as cohesive as HA when implanted. For example, calcium hydroxylapatite (CaHA), which is used for fillers that are designed for volume augmentation in nasolabial folds and marionette lines, are not suitable for use the lips due to its high viscosity and elasticity. Furthermore, with the use of CaHa, there is an increased potential for the development of nodules or lumps that are not reversible.[2] One of the reasons why HA-based dermal fillers have become many aestheticians’ favorite type of filler is that unlike other injectables, these fillers can be reversed through the use of hyaluronidase.[3]
The Required Tools and Techniques
When it comes to implanting HA-based dermal fillers, a sharp needle or a cannula will suffice. Deciding between the two instruments is a matter of weighing both their pros and cons. Ultimately, however, one’s respective comfort level with each tool and their suitability for the targeted area should be the deciding factors when determining which tool to use.
What is most important, however, is understanding what kind of treatment suits the patient best. Although there are various analytical guidelines for facial proportions and mathematical techniques have been established, they are not necessarily applicable to all. A good practitioner-patient relationship is essential for achieving an optimal result.
Needle
For lip treatments, it is wise to prepare the HA filler with an analgesic with vasoconstricting properties to reduce the chances of any potential intravascular injection. Use a 30G needle and at least 2cc of lignocaine with adrenaline. [4] Make 34 injection points along the gingival mucosa and the lip junction.
With a sharp needle, run the filler along the vermillion border. From one injection entrance, treat the entire quarter of the lip. The entry points of a lip injection through the vermillion border, and lip injections are done for a number of reasons, including restoring lost lip volume, eliminating perioral lines and rhytids, recontouring the mouth angle, and/or enhancing the philtral columns.[5][6]
The average amount of volume required for an injection of a HA-based dermal filler via a needle is around 12cc, but more filler volume can be used to replace lost volume. It is ideal to inject only as required so as to reduce any chances of bruising or swelling. You may also perform this treatment along with nasolabial folds and marionette lines correction. [6]
Cannula
With the use of cannulae to treat the lips, there is a lower risk of vascular compromise or injury. [7] However, in certain areas that are highly resistant to the passage of cannulae, there is a higher chance of vessel injury occuring. For example, the rhytids in the vermillion borders and perioral area are not easily effaced with a blunt cannula. To avoid tissue resistance, it is better to deposit the filler in a deeper layer, but this requires more volume to be used. A 25 or 27G cannula is ideal for patients who are worried about the risk of swelling and bruising. [6]
When it comes to lip injections, an 18G cannula is only effective for minimal fat transfer to the lips as part of a full-facial fat transfer routine. However, fat transfer is not a common method used for lip augmentation, especially as an isolated treatment. Rather than spending time harvesting fat, turning to filler in a syringe is more cost and time effective. [6]
Lip Dermal Filler Complications
The common side effects of dermal filler injections into the lips are, like other aesthetic injections, mild redness, swelling, bruising and tenderness; these usually subside within a matter of days. In some cases, complications such as fibrosis, inflammatory granuloma, infection, hematoma, filler migration, and thromboembolism may occur. One of the most severe and highly feared side effects of injections of HA-based dermal fillers is vascular compromise as a result of accidental intra-arterial injection or vascular compression. [7][8]
Contrary to beliefs, it is easy to minimize the risk of these complications. The following measures can be taken in order to reduce the prominence of any post-injection adverse effects: [9][10]
- Use a blunt cannula where necessary or if possible.
- Prepare the area with local anesthesia and adrenaline for analgesic effects and vasoconstriction.
- Before injection, aspirate the needle or cannula used.
- Use low pressure for the injection.
- Instead of injecting a large bulk of volume, inject small aliquots of filler.
- Monitor any presence of transient tissue blanching. This could indicate the possibility of vascular compromise.
- Include hyaluronidase in the emergency kit, as this can help dissolve any hyaluronic acid-based dermal filler.
Proper injection techniques can also help achieve optimal results. To avoid poor and unsatisfactory outcomes, keep these tips in mind: [6]
- Do not overcorrect or overfill.
- Plan out the augmentation in accordance with the principles of facial balance and harmony. If possible, treat other perioral regions to balance volume.
- For lips, use HA fillers that have a fine particle size. This can help keep the lips plump and supple without causing bruising.
Lasers for Lip Treatment
Non-ablative lasers are in lower demand simply because there are limited uses for them in the lip and perioral area. Furthermore, with rapid technological advancement in nonsurgical aesthetic treatments, other modalities have offered more options.
However, this treatment can still provide excellent results, although at times it may be unpredictable. Laser treatment is highly suitable for removing any irregular growth on the lips, especially vascular abnormalities or lesions. Long-pulsed lasers can be used to correct venous lakes. Erbium and CO2 lasers are appropriate for skin rejuvenation and treating fine lines, wrinkles, and creases. Skin complexion improvement is another benefit of these lasers. [6]
CO2 lasers have the additional advantage of skin tightening and can be used in both light and dark skinned patients. Full ablative laser resurfacing technique can be used on lighter skin types. Lip blocks or oral sedation is necessary, as it may be painful, and it may cost a longer recovery period. What the procedure entails is the full removal of the upper portion of the dermis to the epidermis. This initiates the stimulation of dermal nerve fibers. [11]
Long term clinical and histological studies on the effects of CO2 lasers have shown that CO2 lasers offer improvements from the mechanical dermabrasion technique, which already has an excellent track record. A prospective study showed that a 950 microsec CO2 laser can be highly effective in the treatment of lip wrinkles in a way that is similar to manual dermabrasion. [12]
In another study, biopsy specimens were taken before the operation and followed at six weeks, six months, and a year after a CO2 laser resurfacing treatment. The study showed that neocollagenesis began to occur at six weeks and progressively increased up to a year. Thus, this study showed that the improvement from this procedure is gradual in nature. [13]
Compared to dermal fillers, ablative lasers should treat the entire cosmetic unit instead of small, isolated areas so as to reduce the chances of demarcating lines. Since each manufacturer make different settings for their products, it is important for practitioners to be well-versed with their laser instrument(s) and understand the energy levels, pulse durations, patterns, and spacings of their own machines. One cannot transfer similar treatment protocols between two different instruments. [6]
Another way to learn about laser resurfacing is to be completely careful and observant to tissue responses and to understand the ideal clinical endpoints. Since each individual has a different skin hydration level and tissue moisture is the main target of CO2 lasers, the use of topical or infiltrative local anesthesia can intervene with the accuracy of the laser pulse. [14] Advise patients to receive regular checkups to monitor the progress of their laser treatment. Different patients may have different tissue responses, even when the same settings are used between two patients.
Following these concerns is the issue of post-operative wound care devised in accompaniment with CO2 laser resurfacing procedures. [15] Wound care includes either open techniques that involve no dressings when wiping the lasered char away or closed techniques that involve the use of occlusive dressings when clearing out the char. However, some clinicians do not bother wiping the char off, as it has the capability to become a biological dressing that naturally flakes off once the skin has fully healed.
Laser Treatment Complications
Laser treatments are useful for treating apparent lesions and patients with a history of anti-viral prophylaxis or herpes labialis. For full laser resurfacing, it is best to prescribe antibiotic, anti-viral prophylaxis and antifungal medication, although these may not be necessary for fractioned resurfacing. [16]
Some of the adverse effects that occur from laser treatment is erythema (redness); bacterial, fungal or viral infection; pain; pigment abnormalities, such as post inflammatory hyperpigmentation (PIH); hypopigmentation; and/or hyperpigmentation. For overaggressive treatments, scarring may occur. [17]
With laser treatments, transient hyperpigmentation is a common side effect, but this can be treated with hydroquinone. Unfortunately, it is impossible to fix hypopigmentation. [14] Other aftercare considerations for the patient include minimizing sun exposure by using sunscreen following the operation. [18]
Other Treatment Modalities
There are various factors that lead to lip alteration, which in turn requires a variety of lip treatments. These treatments include the following:
- A specialized surgical lip-lift procedure intended to restore upper lip extensions that have been affected through natural aging, exaggerated by the pulling force from sagging jowls and neck skin tissue. This exact process should be done while patient is under local anesthesia. Avoid performing lip augmentation at the same time, as this can make the condition worse. [19]
- Perioral rejuvenation using carboxytherapy, skin needling, mesotherapy, and PRP. [6]
- Botulinum toxin for ameliorating dynamic perioral rhytids and lifting sagging or downturned corners of the lips. Use 24 botulinum toxin units on the lip borders and 510 units in each depressor anguli oris. [20]
- PRP can be combined with other therapies, which will reduce the downtime required for laser resurfacing. [21]
For a more thorough procedure, include controls in each case so as to avoid any irregular changes. This should also be done with split-face comparisons.
Conclusion
Each treatment modality and their associated technique(s) have their own advantages and disadvantages when used for lip augmentation, rejuvenation, and restoration. Regardless of modality and technique(s) employed, perform an assessment of the patient and have a thorough patient management system. Consultation is required to establish the patient’s motivation(s) and expectation(s), their tolerance, their worries about the recovery process, and their pain scale. Overall, consultation can help to determine the suitable therapy or product, like Belotero, for the patient at hand and ensure a satisfactory result for all parties involved.
References:
- San Miguel Moragas J et al, ‘Systematic review of “filling” procedures for lip augmentation regarding types of material, outcomes and complications’, J Craniomaxillofac Surg, 43 (2015) p.883-906.
- Emer J, Sundaram H, ‘Aesthetic applications of calcium hydroxylapatite volumizing filler: an evidencebased review and discussion of current concepts’, J Drugs Dermatol, 12 (2013) pp.1345-54.
- Pierre A, Levy PM, ‘Hyaluronidase offers an efficacious treatment for inaesthetic hyaluronic acid overcorrection’, J Cosmet Dermatol, 6 (2007), pp.159-62.
- Practical Plastic Surgery, ‘Chapter 3: Local Anesthesia’, Practical Plastic Surgery for Nonsurgeons., 29-44. p. 31.
- Luthra, A. (2015). Shaping Lips with Fillers. Journal of Cutaneous and Aesthetic Surgery, 8(3), 139142. http://doi.org/10.4103/0974-2077.167269
- Gheyi, S., ‘Treating Lips’, Aesthetics Journal, (2015). https://aestheticsjournal.com/feature/treating-lips
- DeJoseph LM, ‘Cannulas for facial filler placement’, Facial Plast Surg Clin North AM, 2 (2012), pp.215-20.
- Grippaudo FR et al, ‘Diagnosis and management of dermal filler complications in the perioral region’, J Cosmet Laser Ther, 16 (2014), pp.246-52.
- Beleznay K et al, ‘Vascular Compromise from Soft Tissue Augmentation’, The Journal of Clinical and Aesthetic Dermatology, 7 (2014), pp.37-43.
- Kim DW et al, ‘Vascular complications of hyaluronic acid fillers and the role of hyaluronidase in management’, J Plast Reconstr Aesthet Surg, 12 (2011), pp.1590-5.
- Gaitan S, Markus R, ‘Anesthesia methods in laser resurfacing’, Semin Plast Surg, 3 (2012), pp.117-24.
- Gin et al, ‘Treatment of upper lip wrinkles: a comparison of the 950 microsec dwell time carbon dioxide laser to manual tumescent dermabrasion’, Dermatol Surg, 6 (1999), pp.473-4.
- Rosenberg GJ et al, ‘Long-term histologic effects of the CO2 laser’, Plast Reconstr Surg, 7 (1999) pp.2245-6.
- Goldman MP, ‘The use of hydroquinone with facial laser resurfacing’, J Cutan Laser Ther, 2 (2000) pp.73-7.
- Duplechain JK, ‘Novel post-treatment care after ablative and fractional C02 laser resurfacing’, J Cosmet Laser Ther, 16 (2014), p.77-82.
- Gazzola R, ‘Herpes virus outbreaks after dermal hyaluronic acid filler injections’, Aesthet Surg J, 6 (2012), pp.770-2.
- Metelitsa A, Alster TS, ‘Fractional laser skin resurfacing treatment complications: a review’, Dermatol Surg, 3 (2010), pp.299-306.
- Wanitphakdeedecha R, ‘The use of sunscreen starting on the first day after ablative fractional skin resurfacing’, J Eur Acad Dermatol Venereol, 11 (2014), pp.1522-8
- Waldman SR, ‘The subnasal lift’, Facial Plast Surg Clin North Am, 4 (2007), pp.513-6.
- Semchyshyn N, Sengelmann RD., ‘Botulinum Toxin a Treatment of Perioral Rhytides’, Dermatologic Surgery, 29(5) (2003).
- Leo MS et al, ‘Systematic review of the use of platelet-rich plasma in aesthetic dermatology’, J Cosmet Dermatol, 23 (2015).